Radiotherapy Technology
Radiation therapy is roughly divided into teletherapy and brachytherapy. In teletherapy, the irradiated region is irradiated from the outside with some distance through the skin (percutaneously). Brachytherapy, on the other hand, involves placing the radiation source close to the tumor, inside the tumor, inside the body, or on the skin.
New radiotherapy location in Wolfratshausen
In October 2022, we opened our new radiotherapy centre in Wolfratshausen!
Where can you have radiation therapy?
In our group of practices, we offer one of the most important therapeutic procedures for the treatment of tumors. Radiation therapy of malignant cancer cells is very efficient because the beams can be directed specifically at tumor cells, while healthy tissue is largely spared.
How does radiation therapy work?
All patients receive a treatment plan individually tailored to their tumour disease. Our team of doctors and radiation physicists choose the most modern treatment techniques and determine the optimal dose of radiation for the patient.
Radiotherapy is used in cancer treatment either alone or in combination with surgery and/or chemotherapy (radiochemotherapy). If it is used before surgery (neoadjuvant), it helps to shrink the tumour to make surgery as minimally invasive as possible. Radiation therapy can also – used after surgery (adjuvant) – help to reduce the risk of relapse.
With radiotherapy in palliative intention, pain and symptoms of tumor diseases can be alleviated.
Functionality of radiotherapy
Radiation therapy uses ionizing radiation or particle radiation to destroy tumor cells. The aim is to stop malignant cells from dividing in order to reduce tumour growth and eliminate the cancer cells as comprehensively and definitively as possible.
In addition to the irradiation of malignant tumors, Radiologie München also offers the therapy of chronic inflammations as well as painful joint and soft tissue diseases with very low doses of radiation.
Treatment techniques in radiotherapy
Radiation therapy works with different treatment techniques – we focus on VMAT, IMRT and SRS.
Dynamic Rotational Irradiation (VMAT)
VMAT (Volumetric Intensity Modulated Arc Therapy) is a further development of IMRT and currently the most advanced irradiation technique on a linear accelerator. The advantages are:
During radiation, the head of the radiation unit rotates around the patient. This allows treatment times of less than 2 minutes instead of 10-20 minutes. The VMAT technique is our standard and we have many years of expertise in physical planning of this treatment.
Intensity Modulated Radiotherapy (IMRT)
Adapting the region to be irradiated to the shape and contour of the tumor with millimeter precision – that is always our goal. In IMRT, the tumor is irradiated from different directions. At the same time, the intensity of individual irradiation fields can thus be varied during irradiation by means of lead lamellae in the emitter head (MLC = Multi Leaf Collimator). The dose can be placed exactly where it is needed to destroy the tumour, while sparing the adjacent tissue and other organs.
Radiosurgical procedure (SRS)
The SRS procedure (Stereotactic Radiosurgery) achieves very high accuracy in combating tumors and metastases. In this process, a high dose is used to effectively target the corresponding area in a few sessions. Even if the finding to be treated is very close to radiation-sensitive organs or is even localized in such an organ, radiosurgery can be used to treat it gently and usually without side effects. Together with the most modern technology currently available, we offer you our many years of experience in this field for your individual high-precision therapy.
Which types of cancer are mainly irradiated?
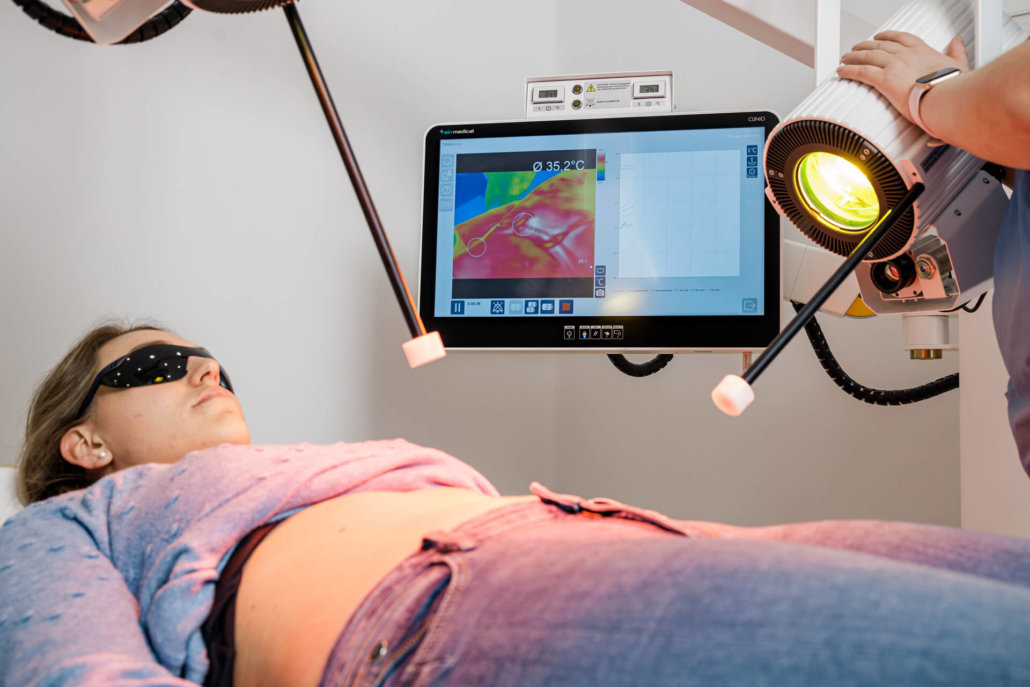
Hyperthermia
In some cases, poor blood supply to the tumor tissue prevents successful treatment. In this case, our specialist team uses targeted heating (hypothermia) to increase the sensitivity of the tumour tissue to radiation therapy.
The combination of hyperthermia and radiation achieves very good therapeutic results, especially with skin and breast cancer. However, the prerequisite is that the tumor is no more than 2 centimeters under the skin. This gentle method only requires weekly treatment over a period of slightly more than one month and is applied before the actual radiotherapy.
This weekly surface hyperthermia with subsequent radiation is only available a few times in Europe – Bavaria-wide currently only in the Radiologie München.
Accompanying measures during radiotherapy
The side effects of radiation can sometimes be more intense – from pain in the tissue around the radiation area to inflammation of the mucous membranes. To reduce these side effects, we use low-level laser therapy and low-level laser acupuncture, among other methods.
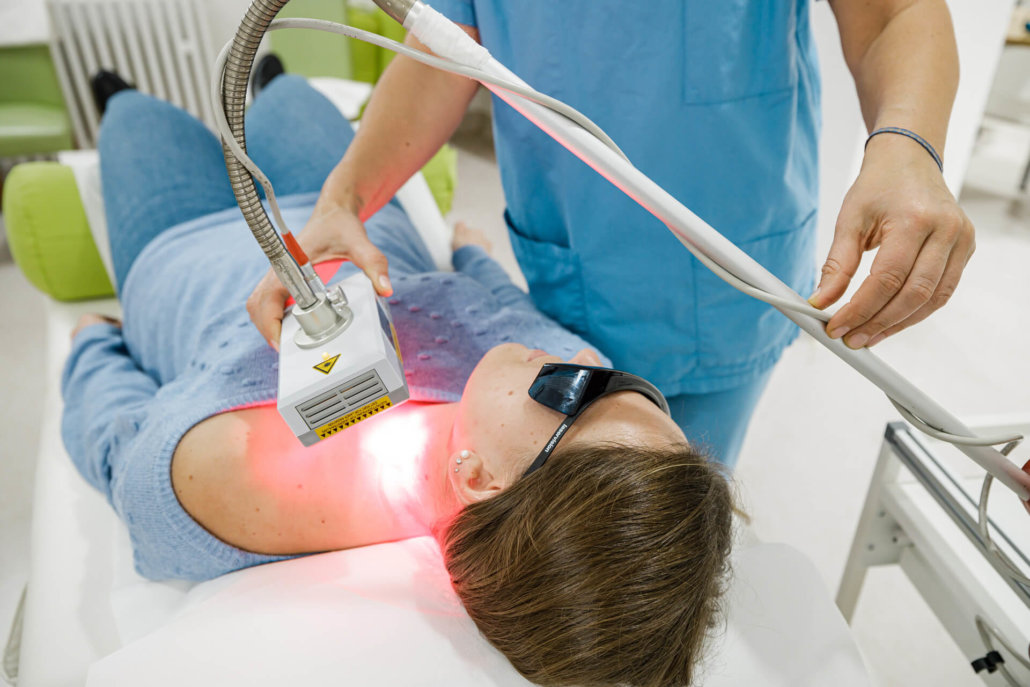
Low-level laser therapy
In low-level laser therapy (LLLT), specific areas are irradiated with a low-energy laser. We treat both areas and specific points directly. Main areas of application in adverse event management:
- Treatment of mucositis (inflammation of the mucous membrane)
- Dermatitis (skin irritation)
- Wound healing disorders
- Pain
The therapy can also be used preventively with the start of radiotherapy to mitigate expected side effects. It is low-stress and free of side effects.
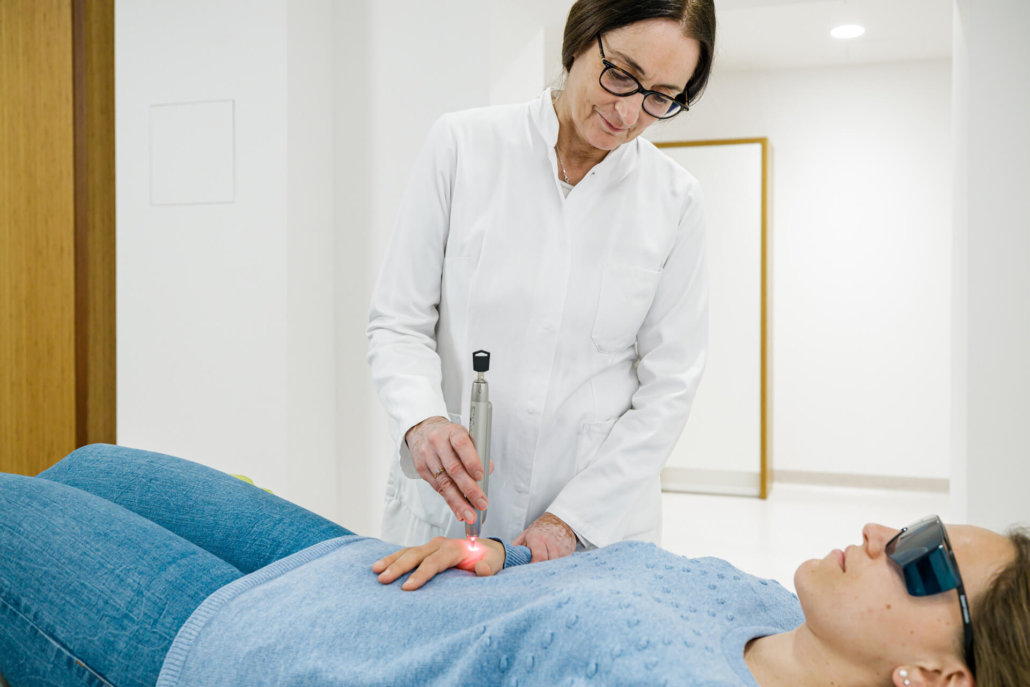
Low-Level Laser Acupuncture
In laser acupuncture, we combine state-of-the-art laser medicine with traditional Far Eastern medicine. However, the acupuncture points are not pricked with a fine needle, but painlessly stimulated or sedated with punctual laser light.
As a regulatory therapy, it can release energetic blockages and contribute to well-being. Typical side effects of radiation or chemotherapy can also be influenced well, in particular complaints such as nausea, fatigue and weakness, anxiety and restlessness. As a complementary/integrative treatment method, laser acupuncture can therefore be very helpful, accompanying radiation therapy.
What should be considered before radiotherapy?
Before your first radiotherapy session, you will have a detailed consultation with your doctor. During this consultation, you will be informed about your treatment plan. In addition, the details of the treatment will be discussed with you, as well as what you need to pay attention to on the day of the treatment. The doctor will tell you whether the treatment will take place on an outpatient or inpatient basis, what documents you need to bring with you and who you can contact if you feel worse after the treatment.
Usually, you do not have to give up eating or drinking before the treatment. Exceptions are made for radiotherapy to the stomach or intestines, or for some forms of brachytherapy. In these cases, you must not eat or drink anything after 10pm the day before. You can get more detailed information about this in advance when you talk to your doctor.
Can you continue to take your medications?
Please tell your doctor in advance what medications or supplements you are currently or regularly taking. Some medications must be temporarily discontinued or replaced because they may have an impact on radiation therapy effectiveness.
What should you wear for radiation therapy?
In general, we recommend wearing comfortable clothing. However, clothing and jewelry that are within the irradiation field must be removed before treatment. Make-up and care products are usually unproblematic.
Can I receive radiation if I have a pacemaker or defibrillator?
For electronic devices such as pacemakers and defibrillators, irradiation can potentially affect function. Please inform your physician as soon as possible to clarify whether these devices are in the treatment area.
During the examination, please pay attention to possible symptoms such as palpitations, shortness of breath or dizziness in order to be able to stop the treatment in time.
Can I be irradiated with an artificial joint?
In principle, an artificial joint or prosthesis does not pose a problem during radiation therapy. The prosthesis may need to be included in the treatment plan if it is in the treatment area.
Are there any restrictions for pregnant women?
Pregnant women may only undergo this treatment to a limited extent due to the sometimes high radiation exposure. At certain stages of pregnancy, malformations or developmental disorders may occur in the unborn child. The child would then be at increased risk of developing cancer or leukemia.
If you are or may be pregnant, please discuss this with your radiotherapist immediately. In this case, it is recommended to postpone the therapy until the birth of the child or to consider alternative treatment methods with a lower radiation exposure.
How does radiation therapy work?
Before the treatment of tumor cells can start, preliminary examinations are necessary in order to plan the therapy precisely. In most cases, a computer tomography is performed at the beginning, sometimes additionally a magnetic resonance imaging. Using the image data, the team of doctors and radiation physicists determines and marks the part of the body to be irradiated (irradiation field) and draws up a therapy plan.
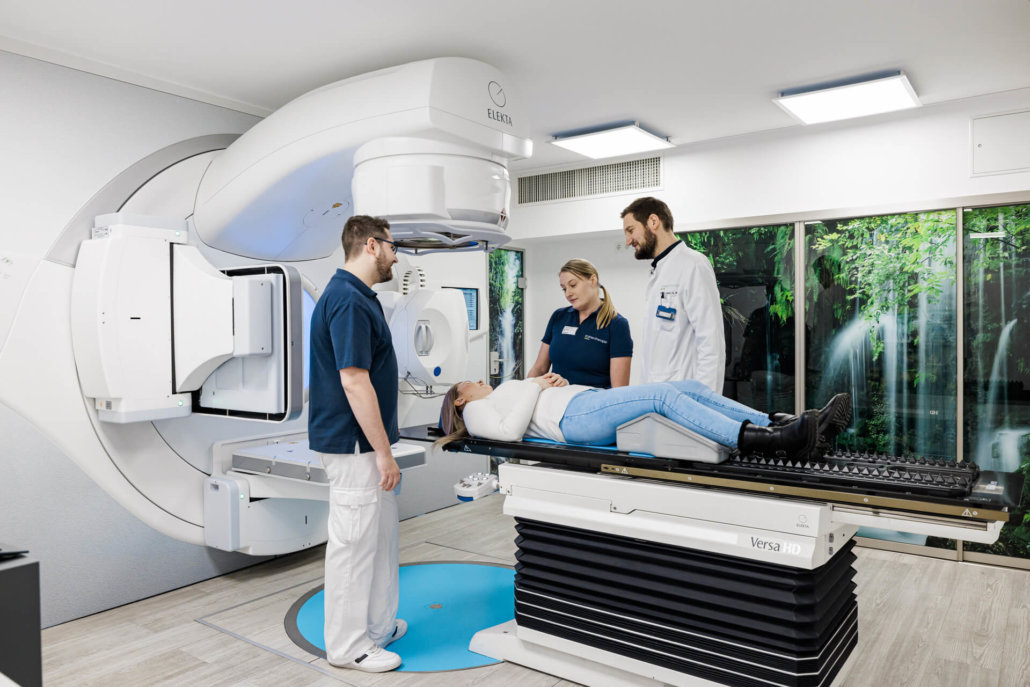
Teletherapy
In order to destroy only the cancer cells during high-energy radiation and to protect the healthy tissue around the tumor, it is necessary not to move the body during treatment. The body parts around the irradiation field are fixed with the aid of positioning aids such as vacuum mats, masks, abdominal presses, etc. In this way, your body moves around the irradiated body part only minimally or not at all, which leads to significantly fewer side effects and radiation damage.
The actual irradiation session is completed after only a few minutes or seconds. The treatment is painless, the rays are neither seen, smelled nor heard. The medical staff leaves the treatment room during irradiation. Through special camera systems and a microphone, the patient is in contact with the treating staff at all times.
Brachytherapy
To best protect healthy tissue and evenly expose only cancer cells to the radionuclide irradiation, the applicators or guide sleeves must be inserted into the body prior to treatment. Depending on the treatment method and body site, local anesthesia or anesthesia is appropriate for this.
As with teletherapy, the individual treatment is over after only a few minutes. The radionuclide is then removed. Depending on the treatment, the guide sleeves remain in the body between irradiations or they are removed. Your medical team will inform you about this in advance.
What are the side effects of radiation therapy?
Radiation aims to slow down cell growth and the spread of cancer cells in the body. Our specialists select the radiation field in such a way that surrounding healthy tissue is spared as much as possible. Despite all sparing, side effects may occur.
Among other things, radiation can affect the blood-forming cells in the bone marrow. Red blood cells are responsible for oxygen transport. If fewer red blood cells are produced, the oxygen supply in the body can be impaired. Therefore, the patient may experience fatigue after the treatment.
White blood cells, on the other hand, are important for the immune system: too few white blood cells can lower the body’s immune defence, making the patient more susceptible to disease. Platelets are responsible for blood clotting. Too few platelets can therefore lead to bleeding.
Irritation of mucous membranes, skin, hair loss
During radiation treatment, mucous membranes of organs and tissues located in the irradiation field are irritated. If the mucous membranes are affected, inflammation, swelling, infection, diarrhea, intestinal discomfort and pain may occur.
Similar to mucous membranes, the skin is also affected during irradiation. Possible consequences are sunburn-like redness or a tightening or itching of the skin in the irradiation field. Sometimes desiccation or scarring can also be observed.
Radiation therapy can cause hair loss. However, in contrast to chemotherapy, only a regionally delimited area of the body is irradiated. Depending on the intensity of the radiation, hair loss may occur at this point.